Chapin White has come up with an explanation for why the United States spends so much more than the rest of the world on health care: private health plans pay wild prices for outpatient care.
White and colleagues have put data supporting that conclusion in apaper distributed by the RAND Corp.
(Related: ‘Surprise Medical Bill’ Witnesses Clash Over Binding Arbitration)
White briefed state insurance regulators on the study findings today, at a session in New York that was organized by the National Association of Insurance Connissioners’ Health Insurance Innovations Working Group.The NAIC started its summer national meeting this weekend in New York.
The NAIC is a group for insurance regulators. Its meeting discussions can shape states’ efforts to write and update Insurance laws and regulations.
White said RAND conducted its research in response to earlier research showing that U.S. residents get about as much health care as residents of other countries but pay much higher prices for the care, and other research showing that most of the gap is due to the high prices private health plans pay.
White’s team looked at the price gap by comparing health care facilities reimbursement data, from states with good data, with traditional Medicare plan reimbursement data.
One thing the researchers found is that private plan payments averaged 241% of Medicare payments for the same care at the same hospitals, up from a private-to-Medicare payment ratio of 236% in 2015.
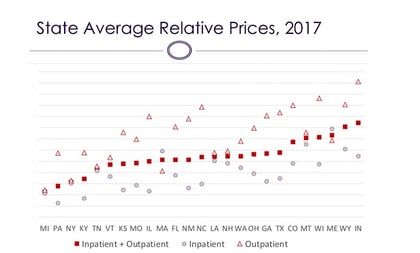
Another thing is that the private plan-to-Medicare spending ratio for facility bills varied wdely from state to state.
The ratio ranged from under 175%, in Michigan, up to more than 275%, in Indiana, with a median between 225% and 250%.
The researchers found that, in most of the states studied, the ratio was much higher for outpatient care than for inpatient care.








 August 03, 2019 at 09:49 PM
August 03, 2019 at 09:49 PM










